-


Academics
Study to Become a Midwife
Our Austin based midwifery program is devoted to presenting a dynamic curriculum meant to assist students in the mastery of midwifery skills. Our approach blends classroom, clinical work, and apprenticeship hours designed to maximize the transition of theory into practice.
Our next term begins the week of July 21th, 2024!
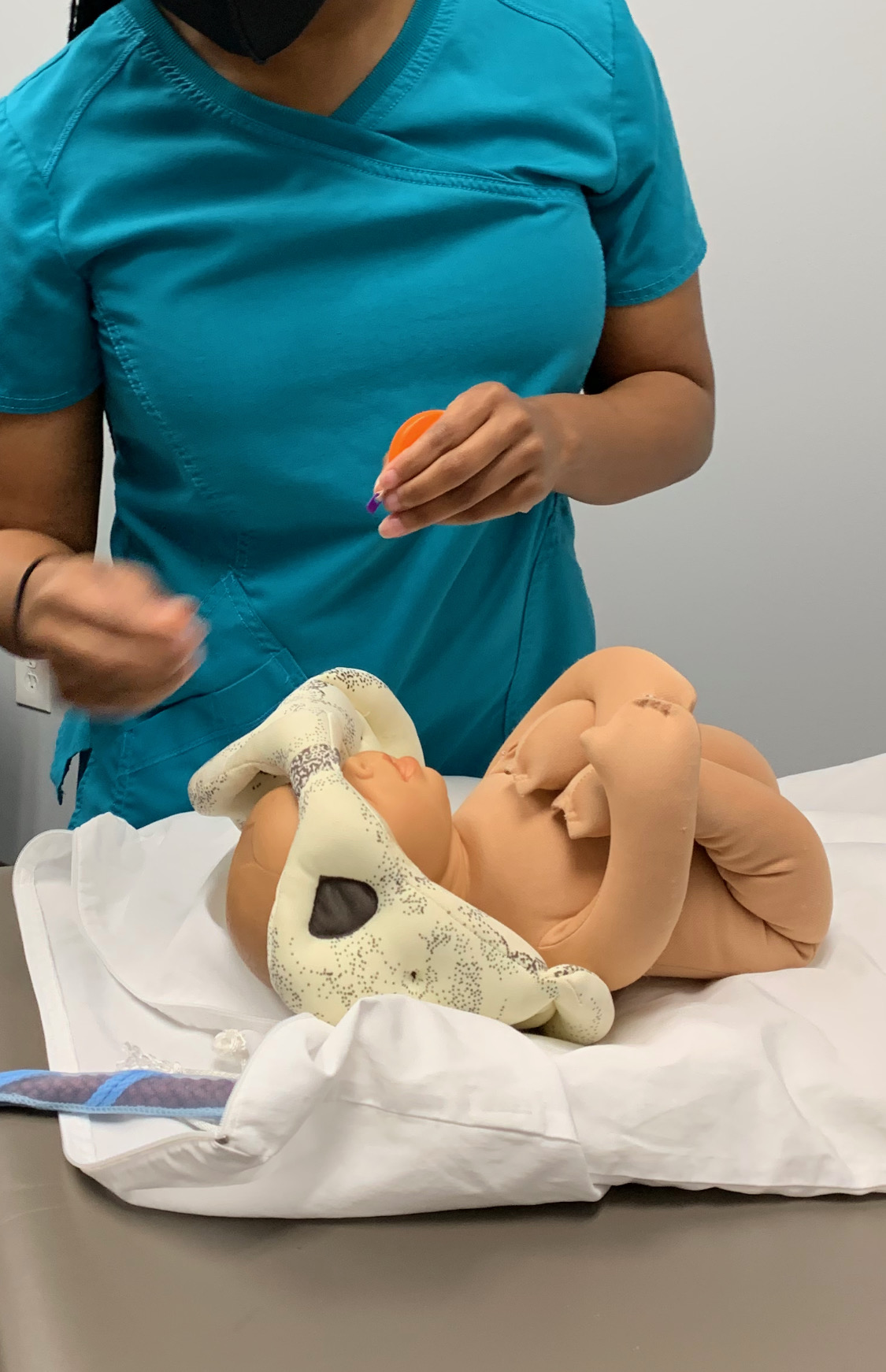
Academic and Skills Development
Students will spend 900 hours in the classroom. Students can expect to spend 2 hours studying outside of class for every hour spent in class. Classes are a blend of skills and academic learning that is both teacher as well as video led. Our students are taught the basics right away - blood draw, vital signs, urinalysis - and they put those skills to work!
- The classroom portion of the program may be completed in 12 - 24 months.
- Clinical training typically takes 24 - 36 months and is completed concurrently with the classroom portion.
Clinical Training / Apprenticeship
Clinical Training includes direct client care through prenatals, labor and deliver, and postpartum. Clinical hours will be a minimum of 1350 hours and must span a minimum of twenty-four months. Students are eligible to apply for apprenticeship after successful completion of their first term. Students have two choices for clinical training:
- Students may apply for an apprenticeship to begin their clinical hours at Beautiful Beginning Birth Center.
- During the first year of study, students may chose their clinic and birth shifts. This may be one or two days a week, or it may be a 24/7 schedule if the student feels that they can balance this with their academic workload. This flexibility allows students to have work-life-school balance.
- During the second year of study, students may apply for an extended apprenticeship with Beautiful Beginning Birth Center. At this point, students are expected to be on-call 24/7 and attend all appointments and births, as well as perform office duties in preparation for the rigors of a midwifery practice.
- Fees are determined by Beautiful Beginning Birth Center's Clinical Director.
- Students may apply for an apprenticeship to complete their clinical hours with a school approved Preceptor-Midwife.
- On call schedule and fees are determined by the Preceptor-Midwife.
It is our belief that a student should attend births and clinics with several midwives throughout her study. This diversity in experiences allows a student to formulate her own philosophy of midwifery and how she would like to practice.

Clinical Requirements
The time it takes a student to complete the clinical requirements is dependent upon the student's availability and competency in performing skills at prenatals, births and postpartums. The time that it takes to demonstrate competency is unique to each individual. A student can expect to attend a minimum of:
- 55 births - In home, birth center and hospital settings,
- 100 prenatals
- 50 postpartums
Students are strongly encouraged to use this requirement as an absolute minimum and to gain as much clinical and birth experience as they can.
Academic Support
Each student is assigned an Academic Advisor when they enroll in the program. The student and advisor meet (either in person or by Zoom) quarterly and students are encouraged to consult with their advisor for academic support, to debrief after a birth, or for any questions that may arise during their training. This person is meant to be a source of encouragement and support to the student.
Classes
1110 Anatomy & Physiology For Midwives
Pre-requisites: None
Co-requisites: None
Hours: 39
A biology based lecture and laboratory combination course designed to allow students to explore the anatomical structure and physiological processes of the human body and how it relates to the field of midwifery. Topics include the basic organization of the body and major body systems.
1200 Medical Terminology
Pre-requisites: None
Co-requisites: None
Hours: 32
The study of medical terminology introduces students to the principals of medical word building – root words, prefixes and suffixes – designed to develop the extensive medical vocabulary used in healthcare. Students will gain an understanding of basic elements, rules of building and analyzing medical words, and medical terms associated with the body as a whole. Utilizing a systems-approach, the student will define, interpret, and pronounce medical terms relating to structure and function, pathology, diagnosis and clinical procedures. In addition to medical terms, common abbreviations applicable to each system will be studied.
1300 Pathophysiology For Midwives
Pre-requisites: None
Co-requisites: None
Hours: 32
This course relates manifestations of disease, risk factors for disease, and the principles for pathology underlying illness and injury.
1910 Intro to Midwifery and the Healthcare Field / Skills I
Pre-requisites: None
Co-requisites: None
Hours: 33
A healthcare based lecture and laboratory combination course designed to introduce students to the field of midwifery and the scope of practice for midwives worldwide and in Texas specifically. This course covers HIPAA and privacy practices, OSHA and blood borne pathogens training, along with universal precautions for safety when practicing in the healthcare field.
2100 - Fertility & Embryology
Pre-requisites: None
Co-requisites: None
Hours: 39
In depth study of the physiology of the fertility cycle as well as natural family planning methods. This course covers birth control methods, their benefits and risks, and human sexuality. Student will explore the development of the fertilized egg from zygote to baby as well as developmental milestones of fetal development.
2200 - Nutrition & Exercise For the Child Bearing Year
Pre-requisites: None
Co-requisites: None
Hours: 32
Nutrition from a holistic, a Western and an Eastern perspective is introduced. Student will gain an understanding of the nutritional requirements for the childbearing year as well as during lactation. Supplements, vitamins, minerals and beneficial herbs will be studied. Exercise physiology, its risks and benefits and modifications for pregnancy and postpartum will be addressed.
2300 – Pharmacology & Ultrasound
Pre-requisites: None
Co-requisites: None
Hours: 32
An introduction to drug class, mechanism of action, basic drug classification of pharmaceuticals a midwife is most likely to encounter in practice. Drug safety is emphasized as well as a detailed protocol for preparing and administering mediations to a woman and her baby. Basics of ultrasound are covered. Students learn what sonographers are looking for while performing an ultrasound, how to read a report, and the legal requirement for interpreting sonography findings. There will be hands on practice for visualizing a fetal heart beat and position of a fetus.
2901 – Skills II
Pre-requisite: 1910 - Intro to Midwifery and the Healthcare Field / Skills I
Co-requisite: None
Hours: 33
This class builds on the foundational skills students learned in Introduction to Midwifery & Healthcare / Skills I class. Students are taught more advanced skills during this class, including skill drills for CPR, first aid, neonatal resuscitation and shock.
3110 – Prenatal
Pre-requisite: None
Co-requisite: None
Hours: 39
The prenatal class introduces antenatal assessment and care of the woman and her fetus. Students learn history taking, physical exam, labs and legal documentation / SOAP Notes. This course addresses assessing maternal and fetal well being; the normal anatomical and physiological changes related to pregnancy; how to determine pregnancy dating, fetal position and growth; how to address the common complaints of pregnancy.
3210 – Diagnostics and Laboratory Investigations I
Pre-requisite: None
Co-requisite: None
Hours: 26
A lecture based course covering the basic laboratory and diagnostic testing most commonly used by a certified midwife. Students will learn the legal requirements for ordering labs and disease reporting, universal precautions and specimen collection. Students will have a strong understanding of what each component of a lab test means and how to interpret the results.
3310 – Research Methods and Statistics
Pre-requisite: None
Co-requisite: None
Hours: 12
Research methods and statistics equips future midwives with the tools to actively engage with and contribute to the expanding body of knowledge in midwifery. By fostering a strong grasp of research principles and statistical techniques, students will be able discerning consumers of research and skills practitioners who utilize evidence-based approaches to enhance the quality of care provided.
3911 – Skills III
Pre-requisite: 2901- Skills II
Co-requisite: None
Hours: 33
A hands on course covering the basics of birth assistant skills and the skills required for monitoring fetal and maternal wellbeing during the antenatal period.
4211 – Diagnostics and Laboratory Investigations II
Pre-requisite: 3210 – Diagnostics and Laboratory Investigations I
Co-requisite: None
Hours: 26
A continuation of 3210 - Diagnostics and Laboratory Investigations I. Students will be assessed through a combination of assignments, case studies, class discussions and critical thinking exercises. These assessments will enable students to demonstrate their understanding of diagnostic testing in the childbearing year.
4310 – Ethics
Pre-requisite: None
Co-requisite: None
Hours: 12
Ethics for midwives is a crucial course that empowers aspiring midwives with the knowledge, empathy, and ethical acumen essential for providing compassionate and culturally sensitive care in a rapidly evolving healthcare landscape. Students will be better prepared to navigate the ethical complexities they will encounter throughout their midwifery careers, ultimately contributing to the promotion of safe, respectful, and holistic midwifery care for diverse populations.
4411 – Abnormal Prenatal
Pre-requisite: 3110 – Prenatal
Co-requisite: None
Hours: 39
A collaborative effort between students and the instructor to write updated, well researched protocols related to pregnancy complications. Using case studies, students will gain an understanding of variations from normal and the signs and symptoms for referral. Collaborative care and transfer of care guidelines will be discussed. At the end of this class, students will have an antepartum protocol document sufficient for use in their practice.
4911 – Skills IV
Pre-requisite: 3911 – Skills III
Co-requisite: None
Hours: 33
This class builds on the skills learned in 3911 - Skills III and introduces students to advanced skills for maternity complications.
5100 – Microbiology
Pre-requisites: None
Co-requisites: None
Hours: 26
This course provides midwifery students with a comprehensive understanding of microbiology essential for their practice. Emphasizing the relevance of microbial biology to maternal and neonatal health, topics covered include the identification, classification, and pathogenicity of microorganisms commonly encountered in obstetric and neonatal care settings. Through lectures, laboratory sessions, and case studies, students will explore microbiological principles, infection control strategies, and the role of microbiota in pregnancy outcomes. Practical skills in microbial identification and antimicrobial stewardship will be developed to enhance clinical decision-making and promote optimal maternal and neonatal health outcomes.
5110 - Intrapartum / Labor & Delivery
Pre-requisites: None
Co-requisites: None
Hours: 39
Assessment of maternal and fetal wellbeing during the intrapartum period. Students will learn to interpret fetal heart rate patterns and respond appropriately to decels, acels and variables. This class teaches the mechanisms of normal labor, describes the updated stages and phases of labor, and the management of a normal delivery. We review normal physiology of labor and birth, how to assess membrane status and contraction patterns. The benefits, risks, contraindications and informed consent for water birth, twins, breech and VBAC will be discussed.
5300 – Lactation / Breastfeeding I
Pre-requisites: None
Co-requisites: None
Hours: 26
Students are encouraged to chose their course in lactation early on. Students that wish to take the add-on class – IBCLE preparation – will need to declare their decision early in their training to begin accumulating the supervised training hours under the supervision of an IBCLC mentor.
For students who choose to take the 5300 - Lactation / Breastfeeding I class - there will be an in-depth review of breast anatomy. Lactogeneis and normal breastfeeding physiology is covered.
5411 – Abnormal Prenatal II
Pre-requisite: 3110 – Prenatal
Co-requisite: None
Hours: 39
A collaborative effort between students and the instructor to write updated, well researched protocols related to pregnancy complications. Using case studies, students will gain an understanding of variations from normal and the signs and symptoms for referral. Collaborative care and transfer of care guidelines will be discussed. At the end of this class, students will have an antepartum protocol document sufficient for use in their practice.
5911 – Skills V
Pre-requisites: 4911 – Skills IV
Co-requisites: None
Hours: 33
A hands on class covering comfort measures and pain management options for labor. Students will practice hand maneuvers for delivery of the baby as well as the management of the third stage of labor. Placental assessment is covered here.
6411 – Abnormal Labor & Delivery I
Pre-requisite: 5110 – Labor & Delivery
Co-requisites: None
Hours: 39
A collaborative effort between students and the instructor to write updated, well researched protocols related to intrapartum complications. Using case studies, students will gain an understanding of variations from normal and the signs and symptoms for referral and transport. Teaches students the proper etiquette for an emergency transfer of care during labor including how to give a proper report to EMS personnel as well as to the receiving facility. At the end of this class, students will have an intrapartum protocol document sufficient for use in their practice.
6501 – Lactation / Breastfeeding II
Pre-requisites: 5300 – Lactation / Breastfeeding I
Co-requisite: None
Hours: 26
Breastfeeding complications, tongue and lip tie and breast health.
6911 – Skills VI
Pre-requisites: 5911 – Skills V
Co-requisite: None
Hours: 33
Hands on practice of emergency skills for both birth emergencies.
7600 – Newborn Care
Pre-requisites: None
Co-requisite: 7700 Postpartum Care
Hours: 39
This class covers everything from APGAR to normal physiologic and anatomic adjustments to extrauterine life, thermoregulation, the comprehensive newborn exam and documentation in the newborn record. State required screenings and testing will be discussed.
7700 – Postpartum Care
Pre-requisites: None
Co-requisite: 7600 – Newborn Care
Hours: 26
This class covers the maternal care schedule for postpartum care. Topics include diastasis, pelvic floor assessment, exercise, nutrition, return to fertility, and family planning options.
7801 – Abnormal Labor & Delivery II
Pre-requisites: 6411 - Abnormal Labor & Delivery
Co-requisite: None
Hours: 39
A continuation of 6411 - Abnormal Labor and Deliver I. This course covers the legality of transports, identifying complications, abruption, hemorrhage, shock, retained placenta, fetal distress and pharmacologic agents.
7911 – Skills VII
Pre-requisites: 6911 – Skills VI
Co-requisite: None
Hours: 33
Hands on practice to estimate blood loss, perineal assessment and repair, and medication administration for the immediate postpartum.
8101 – Business of Midwifery
Pre-requisites: All 1000 – 7000 Level Courses
Co-requisites: None
Hours: 24
The Business of Midwife prepares students to embark on a successful and sustainable midwifery career by providing the knowledge and skills needed to navigate the business aspects of a healthcare practice. Upon completing this course, students will be equipped to create patient-centered, ethically driven, and financially viable midwifery practices that contribute positively to the well-being of clients and the broader community./span>
8201 – Practice Management
Pre-requisites: All 1000 – 7000 Level Courses
Co-requisites: None
Hours: 12
A comprehensive course that equips students with the knowledge and skills necessary to effectively manage and operate a successful practice. Students will gain practice management skills including preparing superbills for the billing company,
8301 – Texas Midwifery Information and Instructor Manual
Pre-requisites: All 1000 – 7000 Level Courses
Co-requisites: None
Hours: 2
This course fulfills the Texas State requirements for training on the Texas Midwifery Information and Instructor Manual, Texas Midwives Law and Texas Midwives Administrative Rules.
8401 – NARM Prep
Pre-requisites: All 1000 – 7000 Level Courses
Co-requisites: None
Hours: 6
Through a combination of assignments, quizzes and case studies, students will be able to demonstrate their understanding of midwifery concepts in preparation for the NARM exam.
99100 – Clinic
Pre-requisites: successful completion of first term
Co-requisites: None
Hours: Minimum 1350
Clinical hours and schedule will vary between clinical locations.
Quarterly peer review - 4 hr
